Adolescent Medicine Update: Oral Contraceptives: Five Vignettes Illustrate Dx and Rx Problems-- and Solutions
Oral contraceptive (OC) pills are frequently prescribed for a variety of clinical purposes. These medications--which contain varying amounts of estrogen- and progestin-based compounds--essentially "override" a woman's innate hypothalamic-pituitary-ovarian axis and frequently help ameliorate the effects of a maturing reproductive system while preventing pregnancy.

Oral contraceptive (OC) pills are frequently prescribed for a variety of clinical purposes. These medications--which contain varying amounts of estrogen- and progestin-based compounds--essentially "override" a woman's innate hypothalamic-pituitary-ovarian axis and frequently help ameliorate the effects of a maturing reproductive system while preventing pregnancy.
This article reviews the clinical effects of hormonal contraception. Five clinical vignettes are presented that focus on diagnosis and management of problems that may occur when teenagers take OCs.
A Quick Review of Oral Contraceptives
The typical OC pill contains a combination of an estrogen (usually ethinyl estradiol) and a progestin. To understand how OCs work, remember that ovulation occurs because the hypothalamus secretes gonadotropin-releasing hormone (GnRH), which stimulates the pituitary gland to produce follicle-stimulating hormone (FSH) and luteinizing hormone (LH). High levels of estrogen and progesterone inhibit secretion of FSH and LH at the level of the hypothalamus (via GnRH) via the pituitary gland. Thus, the body requires sufficiently low levels of estrogen to allow for FSH secretion and follicular maturation, followed by an estradiol surge that prompts secretion of LH to stimulate ovulation (Figure 1).
To prevent follicular maturation, a patient requires consistent, high levels of estrogen to provide feedback inhibition on the hypothalamus (which subsequently inhibits FSH secretion). In addition, high levels of estrogen combined with progesterone effectively inhibit the LH surge, which inhibits ovulation. Therefore, the estrogen and progesterone in OCs provide an exogenous level of inhibitory control to the hypothalamus and pituitary gland. The result is decreased FSH and LH secretion and prevention of ovulation.
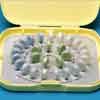
OCs typically come in packages of 21 to 28 pills so that the patient can easily keep track of her menstrual cycle. The 21-day packages require the patient to stop taking pills once all 21 pills have been consumed; after waiting a week (while menses occur), a new package is started. Many adolescents find it less confusing to use a 28-day package (Figure 2). The 7 placebo pills taken at the end of the month allow them to maintain their routine without having to remember to reinstate the regimen the following week.
The estrogen component of most OCs is ethinyl estradiol. Over the past 30 years, the concentration of this hormone has dramatically decreased from that used in initial OC studies. After the patient ingests the pill, the liver provides a significant first-pass metabolic effect such that most of the hormone is metabolized before it reaches its target organs. Most commercially available combination hormonal contraceptive pills contain between 20 and 35 µg of ethinyl estradiol. Patients generally do not notice significant differences in clinical efficacy based on a difference of 15 µg of hormone.
Progestin, the other active component in OCs, primarily binds to progesterone receptors; it may also cross-react with androgen receptors throughout the body. Therefore, androgenic potential is frequently the major consideration when choosing an OC. The progestins, norethindrone and levonorgestrel, both tend to cross-react with androgen receptors. They also displace testosterone from sex hormone binding globulin (leading to an increase in free testosterone levels), thereby providing a fairly strong androgenic effect.
In contrast, norgestimate has decreased androgen affinity and also functions as a 5a-reductase inhibitor. Because of its androgen- minimizing effects, norgestimate may be more appropriate for the adolescent with severe inflammatory acne. Another new progestin, drosperinone (Yasmin) is a spironolactone analog with excellent anti- androgen and anti-mineralocorticoid properties.
OCs are also distinguished by the amount of hormone they deliver throughout the 4-week cycle. A constant rate of estrogen is typically maintained in all of the bioactive pills. In a "monophasic" OC, the progestin concentration remains constant. A "biphasic" or "triphasic" pill has varying progestin concentrations over the first 3 weeks of the cycle. In my experience, multiphasic pills do not provide significant benefit over a monophasic option except in certain scenarios (discussed below).
Adverse Effects
Nausea is a common complaint among patients who start OC therapy. This problem (caused by the estrogen component) usually lasts for a few hours immediately after the pill is taken. I recommend that patient take the medication just before going to sleep. The nausea tends to disappear with consistent use: most patients report that it resolves within 1 to 2 months.
Estrogen-sensitive patients may complain of fluid retention, headaches, intermittent spotting, and/or mood changes. If these symptoms are not severe, then "watchful waiting" or a decrease in the ethinyl estradiol content may suffice. If symptoms are severe, however, consider other contraceptive options.
No discussion of OCs would be complete without mentioning the black box warnings of potential venous thromboembolism. The risk of deep venous thrombosis (DVT) increases dramatically if the patient smokes tobacco or has a history of DVT. Therefore, all patients must be screened for a personal or family history of DVT and counseled about DVT risk before OC therapy is started. Patients who complain of leg swelling, shortness of breath, or chest pain need an immediate workup to determine whether a thromboembolic event has occurred.
Adverse effects of progestin are generally related to the degree of androgenicity described earlier. The more androgenic progestins, such as levonorgestrel, may cause acne, appetite increases (with possible weight gain), male pattern hair loss, and hirsutism. When a patient taking an OC reports these effects, consider switching to an agent that contains norgestimate or drospirenone.
Regardless of whether you actively prescribe combined OCs, you probably encounter adolescents who take these medications for various reasons. The following clinical vignettes illustrate some of the more common issues that may be encountered. I invite you to consider the physiology involved and potential solutions before you read the explanations.
Sixteen-year-old Amelia is concerned about her lack of menses. Her periods began when she was 11, and by age 13 she had regular monthly periods. Over the past year, however, her periods have become irregular. She has not menstruated in over 6 months.
Amelia is an overweight Latina in no distress. She has mild inflammatory acne over her face and chest as well as some hair growth on her chin and naval area. She has mild acanthosis nigricans around her neck.
Amelia denies ever having engaged in sexual activity. Pelvic examination reveals an intact hymen and a urine pregnancy test result is negative.
Results of thyroid studies are normal. LH level is 22 mIU/mL; FSH is 8 mIU/mL. Dihydroepiandrosterone (DHEAS) and testosterone concentrations are both mildly elevated.
As you finish your examination, Amelia blurts out,"Doctor, is there anything you can do about this facial hair? I feel like I am growing a beard!"
What's happening with Amelia? Can anything help her hirsutism?
Amelia probably has polycystic ovarian syndrome (PCOS). This process, characterized by amenorrhea, hirsutism, obesity, and acne, may be caused by abnormal function of the hypothalamic-pituitary-ovarian axis, leading to excessive androgen production in the form of androstenedione and DHEAS. These androgens may be converted peripherally to testosterone, resulting in hirsutism. Insulin resistance frequently exacerbates the condition.
OCs are frequently used to manage PCOS. While OCs probably do not treat the disease, they can ameliorate many of its troubling androgenic symptoms (such as hirsutism and acne). An OC that contains norgestimate would therefore be appropriate; this hormone has low androgen receptor binding affinity and its 5a-reductase inhibition effect results in decreased testosterone production. An OC with drospirenone as the progestin (eg, Yasmin) is another reasonable choice.
Regardless of the progestin you choose, counsel the patient that while the OC may effectively regulate her menses, it may take up to a year of therapy before the hirsutism and acne improve. Other cosmetic approaches such as shaving, waxing, or electrolysis may be considered if the adolescent is distressed by her appearance. An acne management regimen can be prescribed if the patient's skin troubles her.
Amy, 18, has been taking Lo-Ovral for the past 3 years. She initially started taking the pill because of some moderate dysmenorrhea with heavy menses. Since then, she has had normal, regular periods. Over the past 3 to 4 months, however, Amy has experienced breakthrough bleeding and intermittent spotting throughout her cycle. She reports that she has been sexually active only with her current boyfriend of 2 years and that they always use condoms as a form of back-up protection.
Amy's vital signs are normal. Pelvic examination reveals a normal cervix without cervical motion tenderness or adnexal tenderness. You recommend follow-up in 3 days to review lab results.
At the follow-up visit, you tell Amy that cultures for Neisseria gonorrhoeae and Chlamydia were negative. Her hemoglobin and platelet counts are normal; and her white blood cell count is 5000/µL. While Amy expresses relief about these results, she still wants you to do something about the annoying menstrual bleeding.
Assuming that there is nothing physiologically wrong, how might you help Amy's symptoms?
Breakthrough bleeding is a common yet manageable effect of OC use. While it most frequently occurs during the first few cycles of use, spotting can develop later for no apparent reason. The most common cause of breakthrough bleeding in adolescents is inconsistent pill use, but non-hormonal causes of bleeding (such as endometritis, pregnancy, and trauma) need to be assessed.
The adolescent who religiously takes her pills but who experiences this phenomenon may not have the patience to "wait it out until it resolves," as an adult might. For this reason, be sure to let the adolescent know that you hear her concerns.
When breakthrough bleeding develops and persists, consider changing the estrogen and progestin concentrations in the OC. Find out when the bleeding typically begins. If the bleeding begins toward the end of the cycle, there may be insufficient progestin to stabilize the endometrium. A triphasic pill (such as Ortho Tri-Cyclen or Ortho-Novum 7/7/7) with increasing progesterone over the 3 weeks of hormone administration would be appropriate in this scenario. Alter- natively, some practitioners may continue to prescribe the monophasic pill but during the cycle's third week will add in 7 days of the progestin-only "mini-pill" to provide additional endometrial stabilization.
Conversely, if the spotting begins in the 10 days after menses, the problem may be that insufficient ethinyl estradiol is present to stabilize the endometrial lining. An increase in the estrogen content frequently solves the problem. If this approach does not work, try switching to a triphasic pill in which the progestin dose is decreased in the early part of the cycle relative to the estrogen. In this setting, the triphasic OCs may have a clinically observable benefit over the monophasic OCs.
April began taking a triphasic OC approximately 2 months ago. At her first follow-up visit, she has no complaints. For the first 2 weeks, the pills made her slightly nauseous.
April describes a headache she experienced about 2 weeks earlier. She had been watching television when she began to see flickering lights in front of her left eye. This phenomenon lasted for about 10 minutes; within an hour, a pounding left-sided headache developed. April took 3 ibuprofen tablets and fell asleep for a few hours. When she awoke, she felt somewhat better. Now she is worried that she has a brain tumor.
April reports that her mother and aunt get bad headaches that force them to stay in bed.
Is April's headache related to her OC? What would you do next?
April's headache sounds typical of migraine with aura. Patients who are prone to migraine with aura tend to have more frequent headaches (or even have a first headache)when they take an OC. In contrast, OCs may actually help patients prone to migraine without aura.
Patients who have migraine with aura are at significant risk for stroke if they start taking combination OCs. Because migraine with aura is an absolute contraindication to OC use, April will need another form of birth control, such as a progestin-based intervention.
The 2 most common delivery methods for progestin-based contraception are the mini-pills and depomedroxyprogesterone injections. Currently, approved mini-pills contain either norethindrone or norgestrel. They must be taken at exactly the same time every day to maintain their efficacy. Common adverse effects include amenorrhea and menstrual spotting. While probably safe to use in patients having migraine with aura, the mini-pill must be discontinued if symptoms persist (or worsen) while taking the progestin-based contraceptive.
Michelle, 16, has been taking OCs for 2 years. This weekend, she was hospitalized after experiencing fever and vomiting for 24 hours. A complete blood cell count and a comprehensive metabolic panel were ordered.
The aspartate aminotransferase (AST) level was mildly elevated at 41 U/L (normal, 0 to 35 U/L), but the rest of the results were normal. Because of the elevated AST, a hepatitis panel was ordered. Results showed the patient to be anti-HAV IgM-negative, anti-HCV IgM-negative, hepatitis B surface antigen-positive, hepatitis B virus core IgM-negative, and hepatitis B core IgG-positive. Given the positive serologies, Michelle was told that she had hepatitis B and that she should not be taking OCs.
Twenty-four hours later, Michelle's liver function test results were all normal. Her health had improved, and she was discharged. On her follow-up visit to your office, she asks about what birth control options are available for someone with hepatitis.
What do you tell her? Was it appropriate to stop Michelle's OCs?
When active hepatitis B is suspected, it is appropriate to discontinue the OCs. It is not clear, however, whether Michelle really has active hepatitis B. The mildly elevated AST level is probably the result of vomiting and dehydration related to a simple viral gastroenteritis. The hepatitis B serology results suggest that she had hepatitis B and is now a carrier (as evidenced by the presence of the hepatitis B surface antigen).
According to the World Health Organization's guidelines for OC use, a patient who is a hepatitis carrier should not be restricted from using oral estrogen-based contraceptives. However, the patient who is acutely ill with hepatitis A, B, or C (or any other type) must avoid these medications until the infection resolves and any concurrent liver abnormalities normalize. This is because the ethinyl estradiol is primarily metabolized via the liver's cytochrome P-450 system.
Michelle's hepatic function is intact. She does not have active hepatitis. Therefore, she can start a new pill package as soon as her next period begins.
Christine, a 19-year-old college sophomore, comes to see you over her winter break. She has been taking Ortho Tri-Cyclen for the past year and a half to treat moderate inflammatory acne and for birth control. Until the past few months, the OCs did an admirable job of regulating her periods such that she could "set her clock" by the timing of her menses.
Last summer, Christine began to experience symptoms consistent with bipolar depression. Her psychiatrist prescribed carbamazepine, which yielded excellent clinical results.
Christine is now concerned because her last 3 menstrual cycles have become erratic. She has experienced significant breakthrough bleeding at various times throughout her cycle. She does not have abdominal pain or clinical signs of anemia (her hemoglobin level is 14 g/dL), but she is increasingly annoyed with the bleeding. "I'm doing everything right. I take the pill at the same time every day. I eat well and get plenty of sleep. Why can't I just have the normal periods that I used to have?"
Why should Christine suddenly be having these symptoms? What are her options?
When a patient with a mature menstrual pattern experiences more than 1 to 2 cycles of menstrual irregularities, an investigation is warranted. A sexually active adolescent with frequent spotting or breakthrough bleeding could have endometritis from pelvic inflammatory disease. A pelvic examination with cultures and a urine pregnancy test are therefore warranted.
Once infection and pregnancy have been ruled out, other causes of metromenorrhagia must be examined. Often, the contributing causal factor relates to inconsistency in OC administration. Many middle adolescents require some degree of parental supervision (if appropriate) to remind them to take their pill. Even college students may use their medication inconsistently. It appears that Christine has been taking her pills fairly reliably, however.
In this scenario, the introduction of carbamazepine should be a diagnostic consideration. In theory, many anticonvulsants can stimulate the cytochrome P-450 system, thus facilitating the metabolism of ethinyl estradiol in the liver. The effect ranges from breakthrough bleeding to contraceptive failure. Antibiotics such as rifampin or griseofulvin may have similar characteristics and could decrease the hormone levels and their subsequent efficacy.
I must qualify these statements because they are primarily based on long-standing expert opinion and anecdotal case reports rather than controlled trials. In actuality, there is no clear evidence that these medications decrease the hormone levels, increase breakthrough bleeding, or increase undesired pregnancies. Despite this controversy, I would still discuss with patients the potential for decreased OC efficacy when these pills are taken concurrently with other medications that can induce the cytochrome P-450 system. At the very least, the sexually active patient who takes OCs should consider using a back-up (barrier) form of contraception while taking these medications.
If Christine wants to continue to take combination OCs, she might benefit from a pill containing 50 µg of ethinyl estradiol (such as Ovral or Ovcon 50). While the high dose of estrogen in these formularies could be considered excessive for most adolescent girls, the cytochrome P-450 system theoretically metabolizes a significant portion of the estrogen before any clinical effect is noted.
Some adolescent medicine clinicians advocate use of the estrogen patch (Ortho Evra) or the estrogen vaginal ring (NuvaRing) because the absorbed estrogen bypasses the hepatic first-pass metabolism. This may indeed be a reasonable course of action, but currently there are few data to substantiate these options and they should be approached with caution.
Christine could switch to a progestin-based form of birth control, but she will probably lose the acne-treating benefits of the norgestimate/ethinyl estradiol combination. Many progestins actually exacerbate acne because of their androgenic potential. She needs counsel- ing and a birth control option that will minimize the risk of androgenic effects.
References:
Evidence-Based Studies:
ACOG Practice Bulletin 73: Use of hormonal contraception in women with coexisting medical conditions.
Obstet Gynecol.
2006;107:1453-1472.m Calderoni ME, Coupey SM. Combined hormonal contraception.
Adolesc Med Clin.
2005;16:517-537.
Calderoni ME, Coupey SM. Combined hormonalcontraception.
Adolesc Med Clin
. 2005;16:517-537.
Faculty of Family Planning and Reproductive Health Care Clinical Effectiveness Unit. FFPRHC Guidance (April 2005). Drug interactions with hormonal contraception.
J Fam Plann Reprod Health Care.
2005;31:139-151.
Recognize & Refer: Hemangiomas in pediatrics
July 17th 2019Contemporary Pediatrics sits down exclusively with Sheila Fallon Friedlander, MD, a professor dermatology and pediatrics, to discuss the one key condition for which she believes community pediatricians should be especially aware-hemangiomas.
Itchy skin associated with sleep problems in infants
September 27th 2024A recent study presented at the American Academy of Pediatrics 2024 National Conference & Exhibition, sheds light on the connection between skin conditions and sleep disturbances in infants and toddlers, highlighting itchy skin as a significant factor, even in the absence of atopic