2-year-old boy with atopic dermatitis flare on legs
A healthy 2-year-old boy with atopic dermatitis developed intermittent flares of eczematous patches on his legs with dramatic sparing below the sock line following meals. What is the diagnosis?
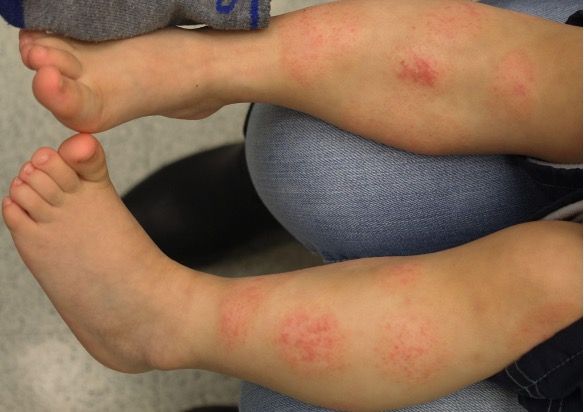
Figure. Legs of 2-year-old boy with atopic dermatitis | Image Credit: Author provided
The case
A healthy 2-year-old boy with atopic dermatitis developed intermittent flares of eczematous patches on his legs with dramatic sparing below the sock line following meals (Figure).
What is the diagnosis?
Atopic dermatitis with flares from some foods.
Clinical findings
Physical examination revealed a dramatic flare of eczema on the patient’s legs, sparing the ankles and feet, which were protected by occlusive clothing. These flares of atopic dermatitis occurred after some meals.
Discussion
Details of the diagnosis
Atopic dermatitis is an inflammatory skin condition often beginning in children under the age of 5 years in the first and second years of life (60% and 21.5%, respectively).1 It presents in a relapsing-remitting pattern and often improves or resolves spontaneously by adolescence.1 The pathophysiology involves a T helper type 2 response, cytokine production (IL-4, IL-5, IL-13), and/or IgE sensitization, resulting in an inflammatory process.2 The reciprocal relationship between a defective epidermal barrier and inflammation results in an “itch-scratch cycle,” which in combination with a filaggrin loss-of-function mutation contributes to a compromised skin barrier.2,3
Atopic dermatitis and food allergy
Children with atopic dermatitis are at a higher risk of developing food allergies, especially in the earlier years of life.4 The initial hypothesis in 1980 postulated that the prevention of atopic dermatitis results from total solid food elimination in the first 6 months of life.5 It is now widely accepted that these 2 events occur in sequence, with atopic dermatitis arising before the development of food sensitization.4 Findings from several studies have confirmed this. Some have reported a 6 times–higher incidence of food allergies in children with atopic dermatitis, an effect that is pronounced the younger a child is at the time of atopic dermatitis diagnosis.3 Other data suggest that of children with temporary skin barrier dysfunction or persistence of atopic dermatitis symptoms, 50% develop a food-specific IgE-mediated reaction and 25% develop positive symptoms on an oral food challenge test.6 Food allergies are a type 2 hypersensitivity reaction and a normal response is maintained by oral tolerance.7 Lack of oral tolerance leads to sensitization to food allergens.7
Adverse food reactions can be categorized as IgE mediated, non-IgE mediated, and mixed-IgE and non-IgE mediated.8 Food allergies are IgE-mediated reactions, occurring within 1 to 2 hours after exposure to a food allergen.8 Atopic dermatitis reactions triggered by consumption of trigger foods are predominantly IgE-mediated eczematous reactions (40%-60%).9 In the absence of an atopic dermatitis flare, they present as urticaria, hives, pruritis, angioedema, morbilliform eruptions, and anaphylaxis shortly after consumption of foods.9 Manifestation of atopic dermatitis flares, an IgE-mediated process, presents with similar symptoms but in a relapsing-remitting fashion.10 The most frequent cutaneous manifestation is acute urticaria, which causes pruritis and a flare-up of the underlying atopic dermatitis.10
Differential diagnosis
Differential diagnoses of atopic dermatitis include contact dermatitis (allergic, irritant), seborrheic dermatitis, psoriasis, infections (impetigo, scabies), metabolic diseases (phenylketonuria, zinc deficiency), malignancies (histiocytosis X, cutaneous T-cell lymphoma), and congenital immunodeficiencies (hyper IgE syndrome, Wiskott-Aldrich syndrome).1
Diagnostic workup
Diagnostic measures of food allergies in atopic dermatitis are reserved for children who either display an immediate reaction after ingestion of a food trigger or experience moderate to severe atopic dermatitis flares despite topical treatment.10 A detailed history is the best first step.10 Other diagnostic tests include skin prick testing, specific IgE testing, oral food challenge, and atopy patch testing.11 Because of the waxing and waning nature of atopic dermatitis, a clinical history has low specificity for non-IgE–mediated reactions that are subtle and delayed.12 In such cases, a trial of an elimination diet for 4 to 6 weeks in addition to a food diary is used for diagnosis.13
Prevention and treatment
For the prevention of food allergen–induced atopic dermatitis in children, parental education on the recognition of symptoms and compliance is vital.14 A diverse diet helps develop tolerance.14 Recent literature data have demonstrated a link between short-duration or nonexclusive breastfeeding and an increased risk of atopic dermatitis.15 For unknown reasons, a cesarean section and assisted delivery are risk factors for atopic dermatitis,16 whereas consumption of a variety of cheeses has a protective effect.17 Administration of the Bacillus Calmette-Guérin vaccine at birth is also linked with a lower risk of atopic dermatitis in children with an atopic predisposition.18
The standard of care for food-induced atopic dermatitis is topical treatment with emollients1,6 and food elimination diets to avoid food allergens.5 Corticosteroids target the inflammatory cascade and repair the defective epidermal barrier.5 Those who remain symptomatic despite topical treatment are candidates for systemic treatment or phototherapy.19 Calcineurin inhibitors, especially in children under 2 years, have received attention in recent years.20 Other lines of research propose early introduction of highly allergenic foods such as cow’s milk, eggs, wheat, and soy to build tolerance.6 The second line of therapy includes food elimination diets whereby suspected food allergens are avoided to symptomatically manage atopic dermatitis5,13; however, this is not without risks. Food elimination diets are associated with nutritional deficiencies and growth restrictions.21 Elimination of cow’s milk in particular is associated with growth delays in height and length, especially in younger children.11,21 This effect can be combated with eliminating a single food item over a period of 2 to 3 months to prevent malnutrition, in addition to dietary supplementation during periods of elimination.21 However, this requires close monitoring and support from pediatric allergists and dieticians.
Latest in treatment
Recent advances in atopic dermatitis and food allergy include precision or personalized medicine, which requires the validation of reliable biomarkers to provide tailored treatment.22 Other therapeutic targets and experimental models for the treatment of atopic dermatitis include various forms of immunotherapy.23 These include food allergen immunotherapy (AIT), oral immunotherapy (OIT), sublingual immunotherapy, and epicutaneous immunotherapy.23 AIT aims to achieve clinical desensitization to build long-term tolerance and prevent future recurrences.23 It has demonstrated the greatest promise for children between the ages of 4 and 5 who had persistent IgE-mediated food allergies to cow’s milk, eggs, and peanuts.23 OIT involves oral administration of increasing amounts of allergen and aims to improve symptoms and the quality of life.23
Patient outcome
In adolescence, severe atopic dermatitis is linked with a higher prevalence of smoking, stroke, cardiovascular disease, inflammatory bowel disease, depression, and anxiety.24 However, most cases of food allergen–induced atopic dermatitis resolve spontaneously with age, especially if the trigger is cow’s milk and eggs.24 Delayed-onset non-IgE–mediated reactions have a better prognosis, and children often develop tolerance by the age of 5.25 Once tolerance has been achieved, outcomes are favorable in those who adopt a diverse diet, which keeps future recurrences at bay.
To read more from the May, 2023, issue of Contemporary Pediatrics®, click here.
References:
- Cartledge N, Chan S. Atopic dermatitis and food allergy: a paediatric approach. Curr Pediatr Rev. 2018;14(3):171-179. doi:10.2174/1573396314666180613083616
- Badloe FMS, De Vriese S, Coolens K, et al. IgE autoantibodies and autoreactive T cells and their role in children and adults with atopic dermatitis. Clin Transl Allergy. 2020;10:34. doi:10.1186/s13601-020-00338-7
- Kalb B, Marenholz I, Jeanrenaud ACSN, et al. Filaggrin loss-of-function mutations are associated with persistence of egg and milk allergy. J Allergy Clin Immunol. 2022;150(5):1125-1134. doi:10.1016/j.jaci.2022.05.018
- Sugita K, Akdis CA. Recent developments and advances in atopic dermatitis and food allergy. Allergol Int. 2020;69(2):204-214. doi:10.1016/j.alit.2019.08.013
- Kajosaari M, Saarinen UM. Prophylaxis of atopic disease by six months’ total solid food elimination: evaluation of 135 exclusively breast-fed infants of atopic families. Acta Paediatr Scand. 1983;72(3):411-414. doi.10.1111/j.1651-2227.1983.tb09738.x
- Graham F, Eigenmann PA. Atopic dermatitis and its relation to food allergy. Curr Opin Allergy Clin Immunol. 2020;20(3):305-310. doi:10.1097/ACI.0000000000000638
- Papapostolou N, Xepapadaki P, Gregoriou S, Makris M. Atopic dermatitis and food allergy: a complex interplay what we know and what we would like to learn. J Clin Med. 2022;11(14):4232. doi:10.3390/jcm11144232
- Calvani M, Anania C, Cuomo B, et al. Non-IgE- or mixed IgE/non-IgE-mediated gastrointestinal food allergies in the first years of life: old and new tools for diagnosis. Nutrients. 2021;13(1):226. doi:10.3390/nu13010226
- Ramírez-Marín HA, Singh AM, Ong PY, Silverberg JI. Food allergy testing in atopic dermatitis. JAAD Int. 2022;9:50-56. doi:10.1016/j.jdin.2022.08.004
- Raveendran R. Tips and tricks for controlling eczema. Immunol Allergy Clin North Am. 2019;39(4):521-533. doi:10.1016/j.iac.2019.07.006
- Sirin Kose S, Asilsoy S, Tezcan D, et al. Atopy patch test in children with cow’s milk and hen’s egg allergy: do clinical symptoms matter? Allergol Immunopathol (Madr). 2020;48(4):323-331. doi:10.1016/j.aller.2020.03.002
- Wollenberg A, Christen-Zäch S, Taieb A, et al; European Task Force on Atopic Dermatitis/EADV Eczema Task Force. ETFAD/EADV Eczema task force 2020 position paper on diagnosis and treatment of atopic dermatitis in adults and children. J Eur Acad Dermatol Venereol. 2020;34(12):2717-2744. doi:10.1111/jdv.16892
- Das A, Panda S. Role of elimination diet in atopic dermatitis: current evidence and understanding. Indian J Paediatr Dermatol. 2021;22(1):21-28. doi:10.4103/ijpd.ijpd_88_20
- Yang EJ, Beck KM, Sekhon S, Bhutani T, Koo J. The impact of pediatric atopic dermatitis on families: a review. Pediatr Dermatol. 2019;36(1):66-71. doi:10.1111/pde.13727
- Napolitano M, Ruggiero A, Fontanella G, Fabbrocini G, Patruno C. New emergent therapies for atopic dermatitis: a review of safety profile with respect to female fertility, pregnancy, and breastfeeding. Dermatol Ther. 2021;34(1):e14475. doi:10.1111/dth.14475
- Gerlich J, Benecke N, Peters-Weist AS, et al. Pregnancy and perinatal conditions and atopic disease prevalence in childhood and adulthood. Allergy. 2018;73(5):1064-1074. doi:10.1111/all.13372
- Nicklaus S, Divaret-Chauveau A, Chardon ML, et al; Pasture Study Group. The protective effect of cheese consumption at 18 months on allergic diseases in the first 6 years. Allergy. 2019;74(4):788-798. doi:10.1111/all.13650
- Thøstesen LM, Kjaergaard J, Pihl GT, et al. Neonatal BCG vaccination and atopic dermatitis before 13 months of age: a randomized clinical trial. Allergy. 2018;73(2):498-504. doi:10.1111/all.13314
- Alexander H, Patton T, Jabbar-Lopez ZK, et al. Novel systemic therapies in atopic dermatitis: what do we need to fulfil the promise of a treatment revolution? F1000Res. 2019;8:F1000 Faculty Rev-132. doi:10.12688/f1000research.17039.1
- Abędź N, Pawliczak R. Efficacy and safety of topical calcineurin inhibitors for the treatment of atopic dermatitis: meta-analysis of randomized clinical trials. Postepy Dermatol Allergol. 2019;36(6):752-759. doi:10.5114/ada.2019.91425
- Eigenmann PA, Beyer K, Lack G, et al. Are avoidance diets still warranted in children with atopic dermatitis? Pediatr Allergy Immunol. 2020;31(1):19-26. doi:10.1111/pai.13104
- Mastraftsi S, Vrioni G, Bakakis M, et al. Atopic dermatitis: striving for reliable biomarkers. J Clin Med. 2022;11(16):4639. doi:10.3390/jcm11164639
- Głobińska A, Boonpiyathad T, Satitsuksanoa P, et al. Mechanisms of allergen-specific immunotherapy: diverse mechanisms of immune tolerance to allergens. Ann Allergy Asthma Immunol. 2018;121(3):306-312. doi:10.1016/j.anai.2018.06.026
- Silverwood RJ, Forbes HJ, Abuabara K, et al. Severe and predominantly active atopic eczema in adulthood and long term risk of cardiovascular disease: population based cohort study. BMJ. 2018;361:k1786. doi:10.1136/bmj.k1786
- Labrosse R, Graham F, Caubet JC. Non-IgE-mediated gastrointestinal food allergies in children: an update. Nutrients. 2020;12(7):2086. doi:10.3390/nu12072086

Newsletter
Access practical, evidence-based guidance to support better care for our youngest patients. Join our email list for the latest clinical updates.
Recognize & Refer: Hemangiomas in pediatrics
July 17th 2019Contemporary Pediatrics sits down exclusively with Sheila Fallon Friedlander, MD, a professor dermatology and pediatrics, to discuss the one key condition for which she believes community pediatricians should be especially aware-hemangiomas.