Another way to manage incessant scratching in children?
What are the skin conditions in which itching becomes the dominant clinical symptom in children?
Another way to manage incessant scratching in children? | Image Credit: © New Africa - © New Africa - stock.adobe.com.

Managing itchy skin, either from acute causes (eg, insect sting or accidental ingestion of allergens in foods or drugs) or chronic causes (eg, atopic dermatitis), can be challenging to parents and physicians. Yet, information on how to manage it has been scarce.
What would be the possible consequences if we allowed children to scratch incessantly? They are obvious. The children will be more irritable, crying often and scratching until the skin starts to bleed. Scratching obviously could not stop pruritus. In fact, the skin lesions would look worse. Further, the lesions would likely develop secondary infection due to staphylococci, Serratia marcescens, or both.
So, what are the skin conditions in which itching becomes the dominant clinical symptom in children? The most common is atopic dermatitis (AD) or eczema, which may start in infancy. In some children, an underlying food allergy could be the culprit. If the lesions become infected, more commonly with Staphylococcus aureus, the itching could worsen. Part of the reason for intensified itching was due to IgE formed against the exotoxin to staphylococci, which has been reported.1,2 Recently, it has been shown that the release of IL-33, an itching cytokine, may contribute to itching as well.3
Currently, there are more medications for the treatment of AD, especially with the availability of new biologics like monoclonal antibody.4 However, pruritus may remain the major symptom and the skin lesions may last longer even as patients begin to respond to the medications. As a result, many parents remain unhappy about the clinical responses of AD to medications.5,6
The next common itching condition is acute or chronic urticaria. Often, the cause of acute urticaria is known (due to insect sting or ingestion of allergic foods or drugs). Removing the cause would help stop the itching. The cause of chronic spontaneous urticaria could be multifactorial. However, in many cases, the cause remains unknown. Therefore, frequent scratching of the urticarial lesions remains the challenge for patients and physicians. Frequent itching is well known to affect quality of life.
The next itchy skin condition we often see in pediatric patients is dermatographia. This is a condition in which the skin becomes overly sensitive to touch or pressure. When skin is scratched or stroked, it causes a red, itchy welt or hive-like reaction. The condition has to do with mast cells under skin that damp out histamine. Symptoms may vary, ranging from mild redness to raised welts like hives. An antihistamine or topical steroid is often prescribed but the effect can vary if the patient continues to scratch.
Another skin condition marked by intense itching is relatively rare: mastocytosis. Many affected children have pigmented skin lesions that help in making the clinical diagnosis. No treatment is available. Reducing scratching will help prevent flare-up of the symptoms. It has been known that preventing children with any of the above skin conditions from scratching is difficult, even with heavy doses of medications.
Three years ago, this author proposed using a “mind-body technique,” teaching children to avoid scratching of skin lesions.7 Our first attempt was trying to control itch in patients with AD, which remains the most common skin disorder in children.
First, we raised with parents the concern that incessant scratching not only worsens existing skin lesions but also increases the chance of superficial infection by Staphylococcus aureus and other organisms that could aggravate the skin lesions with more itching. Further, scratching applies pressure to lesions, which can help release cytokines under skin as in the case of AD.8 Further, incessant scratching would have a negative impact on the psychology of pediatric patients as they could not overcome the urges of the vicious cycle of scratching and subsequent itching. Frequent irritation or behavior changes in those children undoubtedly will make treating skin lesions more difficult.
We first explained to the children the following steps:
- Itching may be the result of “bad energy” stored in the body. We need to get the bad energy out of the body.
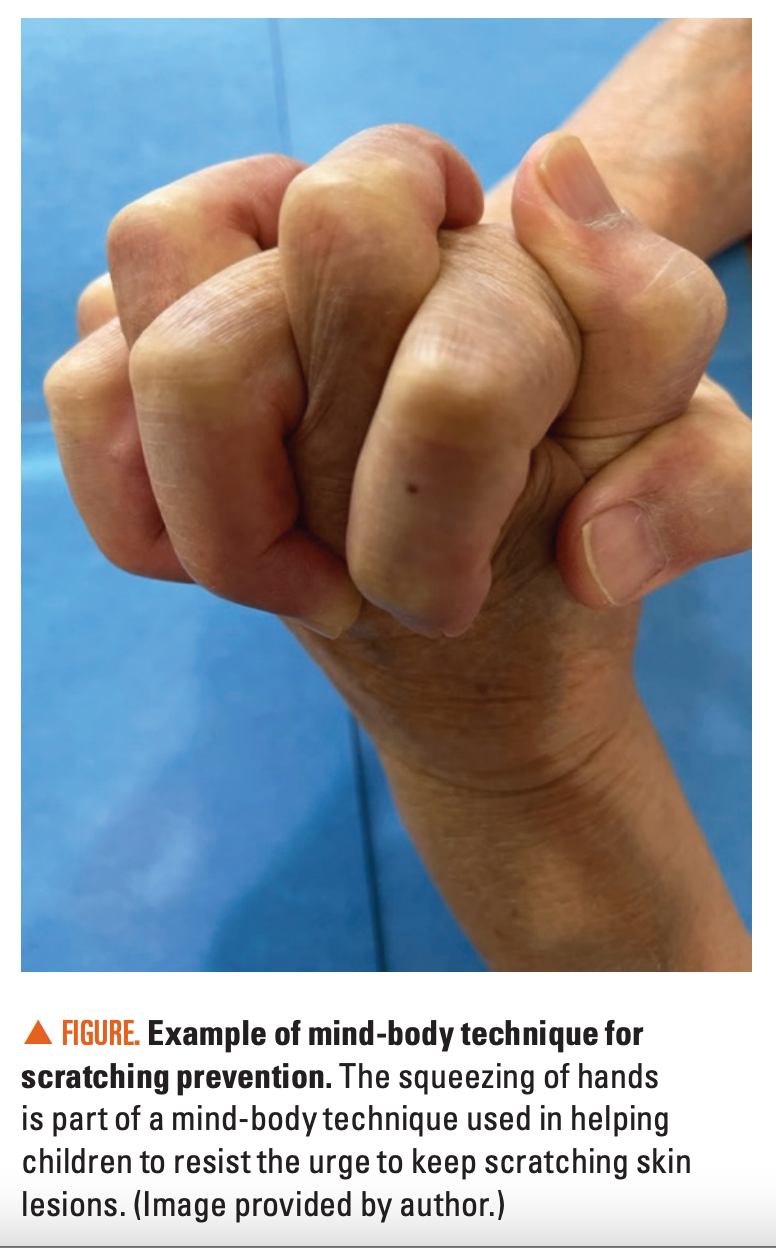
- We taught them how to squeeze their hands as tightly as possible until the skin over the knuckles turned white (Figure).
- At the same time, we let them imagine draining the bad energy from the fingertips as they continued to squeeze their hands.
- The purpose is to let children squeeze their hands for 15 seconds.
- We allowed them to count, “One-one thousand, two-two thousands, three-three thousands…to fifteen-fifteen thousands, after which they relaxed their hands.
- If the urge to scratch returned, we encouraged them to repeat 15-second squeezes.
We let older children imagine that the “bad energy that caused itching” needs to be drained from their bodies, and that the squeezing of hands let bad energy flow from the shoulders to the arms, forearms, hands, and eventually out from the fingertips.
Since our last report 3 years ago,9 we have continued to receive positive feedback from parents on this mind-body technique. They were very encouraged that squeezing of the hands helped children to gain time for medications to work.
We continued to see that nearly 60% of the patients used tropical steroid cream only on an as-needed basis; 50% used oral antihistamine on an as-needed basis. Those results were far better than the control group, which was dependent solely on medications.
Since then, we also introduced the hand-squeeze method to children with chronic spontaneous urticaria, patients with significant dermatographia, or patients with cutaneous mastocytosis. Our overall results showed that among 255 patients with AD, 209 (82%) showed remarkable improvement of the skin lesions with limited scratching. Improvements of lesions with reduced scratching also were seen, as follows: 80% among 64 patients with chronic spontaneous urticaria, 87.5% among 16 cases of dermatographia, and 2 of 3 (67%) patients with cutaneous mastocytosis.
Overall, feedback from those patients was very encouraging. I received no complaint from parents when they adopted this method as part of treating skin lesions. I have also received positive comments from colleagues in dermatology.
On average, after 3 months of using this mind-body technique, we noticed their dependence on oral medication, especially oral antihistamine, steadily decreased. Schoolchildren were happy as the use of oral antihistamine decreased; its accompanying adverse effect of drowsiness also decreased steadily. In turn, their classroom concentration improved. The success rate of reducing scratching in children with AD was higher (near 75%) than for those not using the mind-body technique of squeezing. This was confirmed by the observation of their parents. The children also admitted that they seldom scratched their skin anymore.
As pointed out by Bowen,9 clinicians, rather than solely depending on medications, should strive to create new strategies to treat patients effectively, especially in managing chronic diseases. The addition of mind-body strategy to manage incessant scratching in children could be considered one of those successful examples.
Click here for more from the June issue of Contemporary Pediatrics.
References:
1. Tsutsui H, Mizutani H, Nakanishi K. Contribution of interleukin 18 to the development of infection-associated atopic dermatitis. Curr Probl Dermatol. 2011;41:93-103. doi:10.1159/000323302
2. Bogdali AM, Dyga W, Antoszczyk G, et al. Molecular method of diagnostic allergic sensitization in patients with atopic dermatitis and infected by with Staphylococcus aureus. Przegl Lek. 2016;73(12):818-822.
3. Imai Y. Interleukin-33 in atopic dermatitis. J Dermatol Sci. 2019;96(1):2-7. doi:10.1016/j.jdermsci.2019.08.006
4. Seegräber M, Srour J, Walter A, Knop M, Wollenberg A. Dupilumab for treatment of atopic dermatitis. Expert Rev Clin Pharmacol. 2018;11(5):467-474.
doi:10.1080/17512433.2018.1449642
5. Balkrishnan R, Manuel J, Clarke J, et al. Effects of an episode of specialist care on the impact of childhood atopic dermatitis on the child’s family. J Pediatr Health Care. 2003;17(4):184-189. doi:10.1067/mph.2003.32
6. Mitchell AE, Fraser JA, Morawska A, Ramsbotham J, Yates P. Parenting and childhood atopic dermatitis: a cross-sectional study of relationship between parenting behaviour, skin care management, and disease severity in young children. Int J Nurs Stud. 2016;64:72-85. doi:10.1016/j.ijnurstu.2016.09.016
7. Huang SW. Is there a missing link in the care of atopic dermatitis? a mind-body technique may help stop the habitual scratch. Consultant. 2020;60(4):3-5. doi:10.25270/con.2020.04.00001
8. Paller AS, Kabashima K, Bieber T. Therapeutic pipeline for atopic dermatitis: end of the drought? J Allergy Clin Immunol. 2017;140(3):633-643. doi:10.1016/j.jaci.2017.07.006
9. Bowen JL. Educational strategies to promote clinical diagnostic reasoning. N Engl J Med. 2006;355(21);2217-2225. doi:10.1056/NEJMra054782

Newsletter
Access practical, evidence-based guidance to support better care for our youngest patients. Join our email list for the latest clinical updates.
Recognize & Refer: Hemangiomas in pediatrics
July 17th 2019Contemporary Pediatrics sits down exclusively with Sheila Fallon Friedlander, MD, a professor dermatology and pediatrics, to discuss the one key condition for which she believes community pediatricians should be especially aware-hemangiomas.