- Consultant for Pediatricians Vol 8 No 6
- Volume 8
- Issue 6
May-Thurner Syndrome
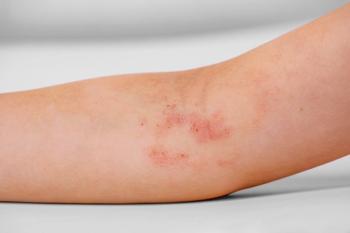
A 14-year-old girl with systemic lupus erythematosus (SLE) was evaluated for worsening left leg pain of 1 week’s duration. A month earlier, she had presented with left knee arthritis and a vasculitic rash; the antinuclear antibody titer was positive. In addition, she had leukopenia, myositis, hypocomplementemia, and mild proteinuria.
A 14-year-old girl with systemic lupus erythematosus (SLE) was evaluated for worsening left leg pain of 1 week’s duration. A month earlier, she had presented with left knee arthritis and a vasculitic rash; the antinuclear antibody titer was positive. In addition, she had leukopenia, myositis, hypocomplementemia, and mild proteinuria. She had responded to treatment with corticosteroids and hydroxychloroquine. She was not taking any other medications.
On examination, the patient had left popliteal tenderness and plethoric engorgement of the left calf. A Doppler ultrasonogram revealed a venous thrombus from the distal femoral vein into the lesser saphenous vein.
Further workup revealed a negative result on testing for lupus anticoagulant, a low-positive result on anticardiolipin antibody studies (IgG, 17 GPL units; IgM, less than 10 MPL units; IgA, less than 12 APL units), homozygosity for the methylenetetrahydrofolate reductase genetic mutation, and normal homocysteine levels. A venogram (injection via the left popliteal vein with the patient prone) revealed a nearly occlusive process in the proximal portion of the left common iliac vein, consistent with May-Thurner syndrome.
This rare anatomic cause of thrombosis was likely responsible for this patient’s deep venous thrombosis (DVT). Although SLE is commonly associated with an increased risk of thrombosis, this patient did not have significantly positive, persistent results on antiphospholipid antibody studies, and her homocysteine levels were normal.
May-Thurner syndrome was anatomically defined in 1957 by May and Thurner1; however, isolated left lower extremity swelling secondary to left iliac vein compression was first described in 1908 by McMurrich.2 May-Thurner syndrome, also known as iliac vein compression syndrome, manifests as left lower extremity swelling, pain, venous stasis changes, and DVT. It results from compression of the left common iliac vein between the overlying right common iliac artery and the lumbar spine, usually at L5. This compression may lead to focal intimal proliferation of the vein, and hence venous stasis in the left lower extremity.2
Although anticoagulation is standard therapy for affected patients, surgical intervention with angioplasty and stent placement is often necessary for recalcitrant thrombi.3 There are no current data comparing treatment modalities for this condition.
This patient was treated with anticoagulation, thrombectomy, and angioplasty of the left common iliac vein at the site of obstruction. The clot was described as hard in texture and thus chronic in nature. She had one recurrence of occlusive DVT. Since then, she has been anticoagulated well. The thrombus completely resolved and has not recurred. Homocysteine levels have remained normal; results of anticardiolipin studies have remained negative.
References:
REFERENCES:1. May R, Thurner J. The cause of the predominantly sinistral occurrence of thrombosis of the pelvic veins. Angiology. 1957;8:419-427.
2. Wolpert LM, Rahmani O, Stein B, et al. Magnetic resonance venography in the diagnosis and management of May-Thurner syndrome. Vasc Endovascular Surg. 2002;36:51-57.
3. Vyas S, Roberti I, McCarthy C. May-Thurner syndrome in a pediatric renal transplant recipient-case report and literature review. Pediatr Transplant. 2008;12:708-710.
Articles in this issue
over 16 years ago
Juvenile Plantar Dermatosis: Readers’ Remediesover 16 years ago
Should Pica Lead to Consideration of Lead Poisoning?over 16 years ago
Traction Alopecia From Atopic Dermatitisover 16 years ago
Vitiligoover 16 years ago
When You Can’t Pry Those Hiding Eyesover 16 years ago
Why Does Facial Rash Flare When Treatment Stops?over 16 years ago
Infant With All-Over Rash, Edema, and Lethargyover 16 years ago
Solution for a Sticky Summer SituationNewsletter
Access practical, evidence-based guidance to support better care for our youngest patients. Join our email list for the latest clinical updates.