Muscle spasms in a 19-year-old male
A 19-year-old male presents to the emergency department (ED) with headache and fever of 4 days’ duration. Six days earlier, his left palm had been punctured by a rusty nail. What's the diagnosis?
A 19-year-old male presents to the emergency department (ED) with headache and fever of 4 days’ duration. Six days earlier, his left palm had been punctured by a rusty nail (Figure). He had cleaned the wound with alcohol and hydrogen peroxide and applied a Neosporin dressing. Two days later, he complained of fever (max 103 °F), headache, abdominal muscle spasms, sweating, and vomiting. Upon questioning, it was determined that his symptoms also included abdominal soreness, shortness of breath, and chills, but he denied rash, dizziness, heart palpitations, chest pain, cough, or any neurologic symptom. Previous medical and surgical history were unremarkable, and the patient had had 5 lifetime doses of DTaP and 1 dose of Tdap 7 years before the injury.
At the ED, the patient was given a bolus of normal saline, intravenous penicillin G, and diazepam and was then admitted to the hospital.
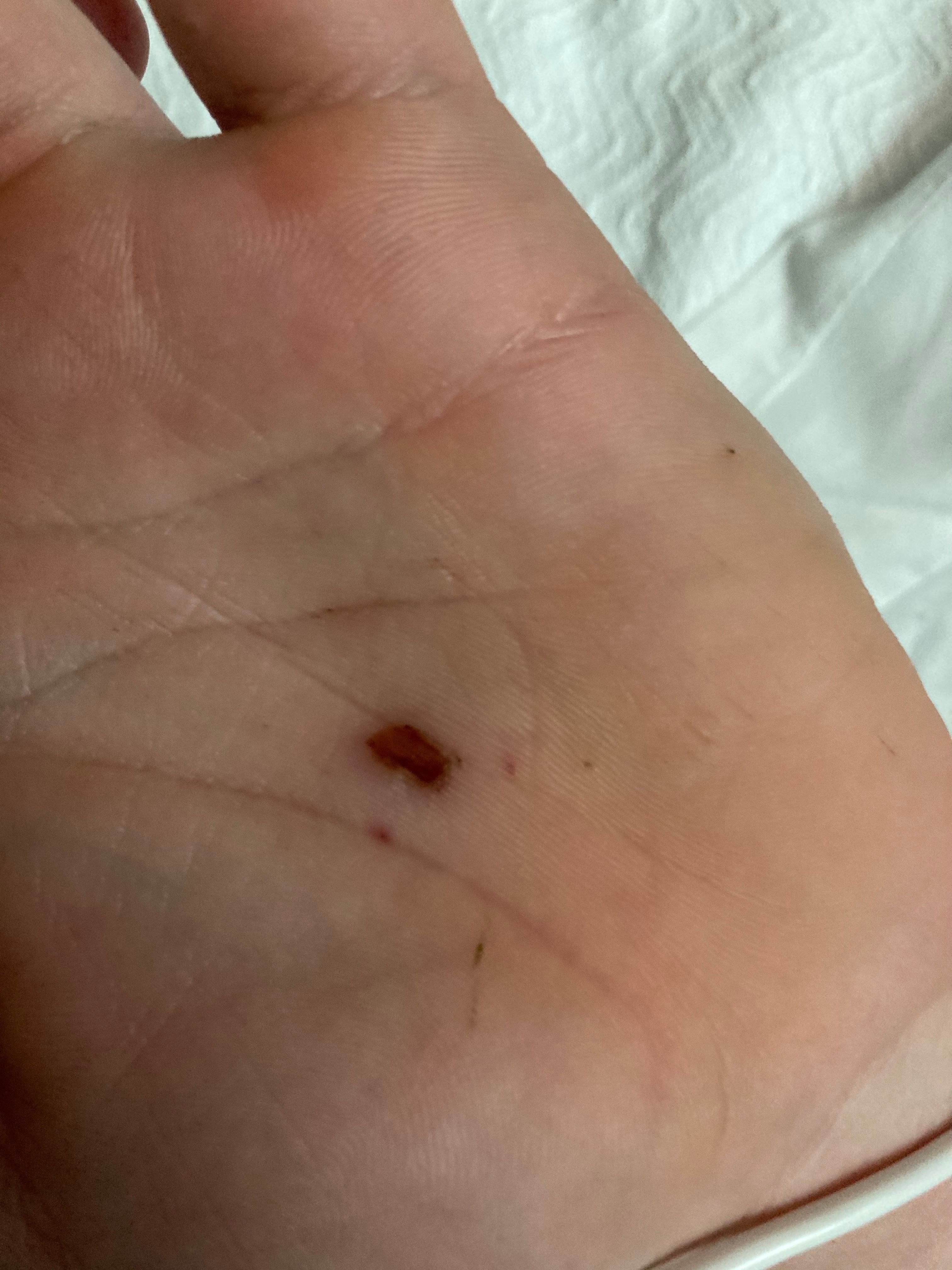
Differential Diagnosis: Tetanus, cellulitis, sepsis, meningitis, seizure activity, and ethanol intoxication were all considered as part of the differential diagnosis. Generalized tetanus was thought to be most likely cause owing to the classic presentation.
Labs/Findings: Upon admission, patient vitals were blood pressure 145/98 mmHg, pulse 137 beats/minute, temperature 100.6 °F, and respiratory rate 26 breaths/minute, with 100% oxygen saturation on room air. The wound was examined and showed no evidence of cellulitis or erythema. A comprehensive metabolic panel (CMP), complete blood count (CBC), lactic acid, blood culture, blood ethanol, magnesium, lipase, lactic acid reflex, prothrombin time (PT)/ international normalized ratio (INR), partial thromboplastin time (PTT), lipase, and troponin were all normal. EKG showed sinus tachycardia, and chest x-ray was unremarkable.
Diagnosis: Given that the puncture wound was not erythematous, draining, warm, or swollen and the labs were unremarkable (ruling out sepsis, cellulitis, meningitis, and ethanol intoxication), the patient was diagnosed with generalized tetanus and hospitalized for observation.
Management: The patient continued to have abdominal muscle spasms for the duration of his stay. He also experienced full-body spasms upon talking, when vital signs were taken, and when he was exposed to changes in lighting. He had difficulty talking, swallowing, and taking deep breaths during full-body spasms, but his oxygen saturation never dropped. The patient never experienced laryngeal spasms. He continued with a normal diet and intravenous fluids and never lost bowel or bladder control. He remained stable, was discharged after 9 days, and advised to follow up with his primary care physician.
Treatment:
The patient was given lorazepam and diazepam as needed for spasms and morphine and ketorolac for pain. He was switched to intravenous (IV) metronidazole for 10 days in place of penicillin G for better tetanus coverage. Enoxaparin was used for deep vein thrombosis prophylaxis and IV ceftriaxone to prevent wound infection and sepsis. Magnesium sulfate was given to prevent autonomic dysregulation and acetaminophen to control fever. Tetanus was treated with intramuscular tetanus immune globulin injection of 500 units and a Tdap vaccination.
Discussion: There are 4 types of tetanus: generalized, local, cephalic, and neonatal, with generalized being the most common.1 The latter is caused by infection from Clostridium tetani, a gram-positive obligate anaerobe found in soil and animal feces. Infection is caused by spores entering the body through a puncture wound or other contaminated injury, especially from rusty nails.2 The spores germinate in an anerobic environment in the wound, such as necrotic tissue, where it forms exotoxin and tetanospasmin, which cause sustained muscle contractions called tetany.2 The toxin goes to the end plate neuromuscular junction, where it travels retrograde to the central nervous system. Once there, the toxin acts on inhibitory Renshaw interneuron cells to prevent the release of GABA and glycine. This leads to the inhibition of inhibitory interneurons and allows neurons to send impulses to muscle cells, causing high-frequency, sustained muscle contractions.1,2 Tetanus has an incubation period of 3 to 21 days, with early-phase presentation consisting of tachycardia, sweating, and restlessness.1 Muscle contractions cause severe muscle spasms like trismus (lockjaw), dysphagia, nuchal rigidity, opisthotonos (backward arching), and risus sardonicus (sustained muscle contractions of the facial musculature resembling a grimace) and compromise the airway, causing dyspnea.1,2 The spasms and hypertonic state can cause extreme pain, exhaustion, fractures, and aspiration.1
Diagnosing tetanus is based on clinical signs and symptoms and tetanus vaccination history.3 Treatment includes tetanus immune globulin, a tetanus vaccine, antibiotics like metronidazole or penicillin G, aggressive wound cleaning, and preparation for airway control and possible intubation. In addition, magnesium sulfate is administered to prevent autonomic dysregulation, and patients should receive medications for pain control (benzodiazepines) and spasms (neuromuscular blocking agents).1,4
According to guidelines from the Centers for Disease Control and Prevention, if a patient with a dirty wound has had 3 or more lifetime doses of a tetanus toxoid vaccine plus a Tdap vaccine more than 5 years prior, a tetanus booster should be administered.3 If the patient has a dirty wound but has had fewer than 3 lifetime doses of tetanus toxoid-containing vaccine, human tetanus immune globulin should be given.3 There were no reported cases of tetanus in the United States in 2018 or 2019 and 26 cases in 2020.5
Patient Outcome: The patient was discharged with home health services and subsequently followed up with his primary care physician to manage the spasms and long-term ramifications of tetanus. He continued to have muscle spasms 5 days after discharge, with myoclonic jerking of the left side of his body. He also showed some gait abnormalities. His primary care physician continued to manage the spasms with clonazepam and cyclobenzaprine.
References
- George EK, De Jesus O, Vivekanandan R. Clostridium tetani. StatPearls. 2022. Accessed January 24, 2023. https://www.ncbi.nlm.nih.gov/books/NBK482484
- Mahan SC, Gladwin M, Trattler B. Bacilus and Clostridium. In: Gladwin MT, Trattler W, Mahan SC, eds. Clinical Microbiology Made Ridiculously Simple. 7th ed. MedMaster Inc.; 2019:58-63.
- Thwaites L. Tetanus. UpToDate. Updated November 18, 2021. Accessed January 23, 2022. https://www.wolterskluwer.com/en/solutions/uptodate/uptodate/take-a-closer-look/sample-topics
- Tetanus–Clinical Information. Centers for Disease Control and Prevention. Updated December 7, 2020. Accessed January 23, 2022. https://tools.cdc.gov/medialibrary/index.aspx#/media/id/231392
- The Global Health Observatory. Total tetanus–number of reported cases. World Health Organization. Updated July 7, 2021. Accessed January 23, 2022. https://www.who.int/data/gho/data/indicators/indicator-details/GHO/total-tetanus---number-of-reported-cases

Newsletter
Access practical, evidence-based guidance to support better care for our youngest patients. Join our email list for the latest clinical updates.
Full case: Infant presents with an asymptomatic pearl-like nodule on the heel
Infant is closely monitored at subsequent well visits and rechecked after 3 months, showed full resolution of the skin lesion over the heel area.
Diagnose this infant with an asymptomatic pearl-like nodule on the heel
Can you diagnose this patient? Take our poll and find out! Then check back for the full case, differential diagnosis, and correct diagnosis.