- Consultant for Pediatricians Vol 9 No 5
- Volume 9
- Issue 5
Is this psoriasis-or something else?
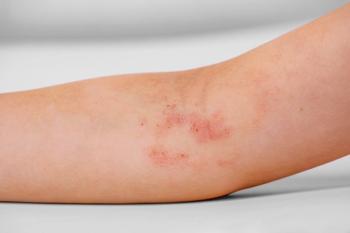
A papulosquamous rash spread from this boy’s head and neck to cover most of his body; however, areas on his trunk were spared.
Case:
A generalized papulosquamous rash developed in this 4-year-old boy over a period of 2 weeks. It began on his neck and head and then spread to his trunk-although some areas on the trunk were not affected. As the rash spread, the skin on his hands and feet became thick and fissured.
At first, the boy's pediatrician suspected psoriasis. What do you think? Are there clinical clues that point to another diagnosis?
Answers on Next Page
He has pityriasis rubra pilaris, suggested by the orange-red color of the scaly papules and the islands of sparing on the trunk.
This young boy has typical pityriasis rubra pilaris (PRP). PRP is characterized by its clinical presentation.
Clinical features of PRP. The condition usually develops rapidly, beginning around the head and neck and progressing to involvement of the trunk and then the extremities. A unique keratoderma develops on the hands and feet; this is characterized by sharp margins and is often referred to as "sandal-like." The primary and characteristic skin lesions are small, follicular reddish yellow scaling papules that coalesce into plaques. These papules/plaques form in such a manner that islands of normal-appearing skin are left- another characteristic sign.
The diagnosis of PRP is usually evident on the basis of the clinical presentation alone. However, a biopsy can be helpful. Biopsy findings of follicular hyperkeratosis and a characteristic pattern of orthokeratosis and parakeratosis will distinguish PRP from psoriasis.
Cause. PRP is an acquired condition with no known cause. However, the rapidity of its development and its frequent occurrence following an infectious illness suggest that it is a reactive phenomenon.
Types of PRP. After 35 years of studying PRP, Griffiths identified 5 types, distinguished by age at onset and clinical presentation (Table).1 The most common variant in children ("circumscribed juvenile" type) is localized to the palms, soles, elbows, and knees; it resolves spontaneously, usually in the late teens. This child has the "classic juvenile" type; the likelihood of his skin clearing within a year is approximately 50% and within the next 3 years, about 80%.
Treatment. This patient's PRP was managed with emollients and an occasional short course of antistaphylococcal antibiotics. This approach was not my first choice; however, after his parents read the literature I provided, they were eager to see whether his condition would remit spontaneously. Over the next 10 months, the child's skin progressively cleared, and he now has minimal residual disease of the palms and soles.
I had planned to start systemic retinoid therapy (which is the systemic treatment of choice) if his PRP had not stabilized after a month of more conservative therapy. This was not required-and I was taught by my patients once again.
References:
REFERENCE:1. Griffiths WAD. Pityriasis rubra pilaris: the Scarlet Pimpernel. Dowling Oration. Liverpool, England: Royal College of Physicians; March 2003.
FOR MORE INFORMATION:
• Allison DS, El-Azhary RA, Calobrisi SD, Dicken CH. Pityriasis rubra pilaris in children. J Am Acad Dermatol. 2002;47:386-389.
Articles in this issue
almost 16 years ago
What Caused This Breast Lump?almost 16 years ago
When to Start Talking About Sex? Earlier Than You May Think!almost 16 years ago
Home Alone: At What Age Are Children Ready?almost 16 years ago
Nevus of Otaalmost 16 years ago
Complicated Cutaneous Anthraxalmost 16 years ago
Newborn With Abdominal Mass and Distentionalmost 16 years ago
Gunshot Victims With Embedded Fragments: Check for Leaching Leadalmost 16 years ago
Rashes and Fever in Children: Sorting Out the Potentially Dangerous, Part 4Newsletter
Access practical, evidence-based guidance to support better care for our youngest patients. Join our email list for the latest clinical updates.