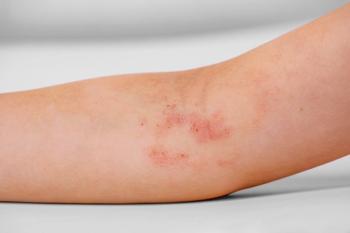
Case 3 Continued: Impressions
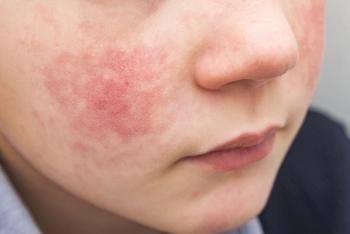
Expert pediatric dermatologists provide impressions on the case of a 12-year-old girl with atopic dermatitis.
Episodes in this series

Joshua Zeichner, MD: Let’s open this up to the entire group and talk about this case. What are your initial impressions?
Elizabeth Swanson, MD: I want to make her better ASAP.
Raj Chovatiya, MD, PhD: And then some. That’s a lot going on in 1 case. Unfortunately, it’s probably similar to stuff we’ve all seen before. Cases like this break your heart because this is everything we talk about. It’s the full burden of disease: the mental health, the social aspect, the actual health, the polypharmacy—everything top to bottom.
Brittany Craiglow, MD: I’m wondering what took her so long to get to dermatology. In some places, there’s poor access. But also, pediatricians often feel either that nothing has helped their patients, so they send fewer patients, or that they’ll grow out of it eventually. When we see patients like this, part of our job is to make sure our letter gets back to the pediatrician, or to call them and say: “There are options now. If you ever have a kid like this, please call me. I don’t want them to suffer.” Because these kids shouldn’t be floating around out there. They need to see somebody who can treat them appropriately.
Raj Chovatiya, MD, PhD: It’s tough across ages when the original gatekeepers are saying this is nothing or just a skin thing and not a big deal, or that there probably isn’t much you can do after lotions and potions and stuff. Both of those are huge gaps in education. Obviously, that’s one problem. But then there’s also the fact that you’re left with patients swirling around the ether and not making it to a place where they can get better.
Elizabeth Swanson, MD: Then when the discussion begins about how to help her and how to fix this, she’s 12, so there are options that exist for her above and beyond topical corticosteroids, TCIs [topical calcineurin inhibitors], and crisaborole. She’s now eligible for topical ruxolitinib, although that’s approved for less than 20% body surface area. I forget if they mentioned the exact body surface area in the clinical vignette. That might be an issue for her, because it seems she has pretty bad atopic dermatitis. Then I’d have a good discussion about dupilumab. I’d also probably include in the discussion a little about upadacitinib, which is approved down to the age of 12. I’d hash out all the choices and do some shared decision-making with the patient and her family and find a way to make this better for her.
Joshua Zeichner, MD: All of you had a gut reaction or a knee-jerk reaction that we need to get this child better right away. But for each of you, what’s your opinion? Are we going to systemic medications right away? Are we adjusting her topicals? What’s your approach in putting together a treatment regimen for this patient?
Raj Chovatiya, MD, PhD: I love how Lisa laid it all out there. I very much love doing the same thing as well. Because in many ways, it’s a bit like a “Choose Your Own Adventure” book, because you don’t know what’s important for the individual patient and their family, what they rank as risk vs not risk, or what the route is. Rather than making that decision for them, I like to make them an active participant in the process.
In this circumstance, as Lisa put it, an oral therapy could definitely be valid. This patient had an oral systemic medication previously, so that’s theoretically a possibility. The biologic is another great possibility. Topicals are another possibility as well. But in this circumstance, without knowing much else about the body percentage area, moderate, etc, a systemic oral therapy is definitely warranted, given the huge burden of disease that we see here.
Vikash Oza, MD: In terms of the systemic [therapy] available to them, probably for most of us, where we’re practicing, it’s going to be dupilumab because they haven’t failed a systemic and that’s on the indication before something like upadacitinib, which theoretically would be available to her if she had failed something like dupilumab. That’s the balance that you weigh as the clinician. But clearly, this is somebody who’s greatly impacted in terms of their quality of life. It clearly is past that threshold. I’ll start patients on a systemic the first time I meet them. It isn’t the majority. The majority is sometimes reassessing and seeing compliance with short-term follow-up. When patients have a very clear story of failed therapies and [are] struggling, sometimes we start a systemic therapy off the bat.
Joshua Zeichner, MD: Take me through your conversations with the patients on the impact of atopic dermatitis on quality of life, especially in someone like this, who’s suffering so much.
Vikash Oza, MD: It’s acknowledging that what they’re experiencing is something that we see experienced by many children with moderate to severe eczema. It’s one of the comorbidities, just like a food allergy or asthma. That’s true of so many of our conditions, when we’re talking about a patient who has hidradenitis suppurativa or alopecia areata. We expect this to have a big impact on you, and in terms of your quality of life. The experience that she’s had isn’t her fault. Her scratching isn’t her fault. Her lack of compliance isn’t necessarily her fault either, when she’s had a disease where she’s had suboptimal care and hasn’t responded so well.
Normalizing that aspect is important because it helps them realize they’re seeing the burden of the disease in their own child. Hopefully, with the right therapies, they’ll see that they aren’t seeing it as much. But there’s also a big role for psychiatric care and mental health support. We think these medicines will drastically improve that, but children who have been suffering from these things can have that mental health aspect across multiple axes in their life, and having support there is important. Normalizing that that’s also a relationship that benefits children with chronic disease is also helpful.
Transcript edited for clarity