- Consultant for Pediatricians Vol 10 No 1
- Volume 10
- Issue 1
MRSA Abscess Attributed to Spider Bite
The family of a 3-year-old girl was concerned about a painful lump in her right palm that they suspected was the result of a spider bite.
The family of a 3-year-old girl was concerned about a painful lump in her right palm that they suspected was the result of a spider bite. The lesion had developed 2 days earlier and had worsened despite treatment with oral cephalexin. The child had no systemic complaints and no sick contacts.
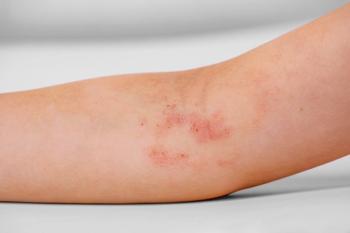
The 4 × 3-cm, dome-shaped abscess in the right palm had a central area of discoloration and mild surrounding erythema. It was tender and fluctuant on palpation. The right hand was mildly edematous, with no lymphangitis. Distal neurovascular status was intact. Remaining physical findings were unremarkable.
Because of the reported high prevalence of methicillin-resistant Staphylococcus aureus (MRSA) among patients with community-associated skin and soft tissue infections,1 treatment with intravenous clindamycin was started, and the abscess was incised and drained. Culture of the wound was positive for MRSA sensitive to clindamycin.
Spiders have long been held responsible for causing a variety of skin lesions, even though in most cases a spider is neither witnessed nor collected.2,3 Lesions falsely attributed to spider bites are usually community-acquired MRSA infections. These infections are often mistaken for necrotic arachnidism because of their similar appearance. Thus, it is important to consider MRSA infection in patients who report spider bites.
S aureus is commonly carried on the skin and in the nose of healthy persons. For unknown reasons, it can suddenly turn against its host and infect the skin. It is a highly virulent pathogen by virtue of its toxins, including exotoxin, leukocyte, and exfoliative toxins. S aureus infection most often affects the skin or soft tissue, although it can cause more serious systemic illness, bacteremia, or death. Close skin-to-skin contact, openings in the skin (cuts or abrasions), contaminated items, poor hygiene, and crowded living conditions all contribute to the spread of MRSA. Standard precautions, such as keeping the lesion covered with a clean and dry bandage, practicing good hand hygiene, and avoiding the sharing of contaminated items, can limit the spread of infection1 and prevent secondary transmission among family members.4
Unlike MRSA infections acquired in the hospital, those acquired in the community are not multidrug-resistant and can usually be treated adequately with clindamycin, trimethoprim/sulfamethoxazole, or linezolid.5,6
After discharge, this child completed a course of oral clindamycin therapy. At 1-week follow-up, she was asymptomatic and had appropriate wound healing.
References:
REFERENCES:
1. Moran GJ, Krishnadasan A, Gorwitz RJ, et al. Methicillin-resistant S. aureus infections among patients in the emergency department. N Engl J Med. 2006;355:666-674.
2. Isbister GK. Necrotic arachnidism: the mythology of a modern plague. Lancet. 2004;364:549-553.
3. Vetter RS. Myths about spider evenomations and necrotic skin lesions. Lancet. 2004;364:484-485.
4. Gross-Schulman S, Dassey D, Mascola L, Anaya C. Community-acquired methicillin-resistant Staphylococcus aureus. JAMA.998;280:421-422.
5. Frank AL, Marcinak JF, Mangat PD, et al. Clindamycin treatment of methicillin-resistant Staphylococcus aureus infections in children. Pediatr Infect Dis J. 2002;21:530-534.
6. Marcinak JF, Frank AL. Treatment of community acquired methicillin-resistant Staphylococcus aureus in children. Curr Opin Infect Dis. 2003;16:265-269.
Articles in this issue
about 15 years ago
Flank Pain, Decreased Urine Output in Young Boyabout 15 years ago
What Rash Consists of These Brownish Macules?about 15 years ago
Pityriasis Rosea in Dark-Skinned Childrenabout 15 years ago
Hydrocephalus Secondary to GBS Meningitisabout 15 years ago
Observation and Documentation Still the Foundation of Medical Practiceabout 15 years ago
Assigning Blame in Medicine: Where Are We Headed?about 15 years ago
Positional Plagiocephaly, Part 2: Prevention and Treatmentabout 15 years ago
X-Linked Ichthyosisabout 15 years ago
Systemic Lupus Erythematosusabout 15 years ago
Toddler With Chest Pain, Trouble Breathing, Cough After Heart SurgeryNewsletter
Access practical, evidence-based guidance to support better care for our youngest patients. Join our email list for the latest clinical updates.