Treatment Selection in Pediatric AD
Angela Lamb, MD, shares her approach to treatment selection for pediatric patients with AD.
Episodes in this series

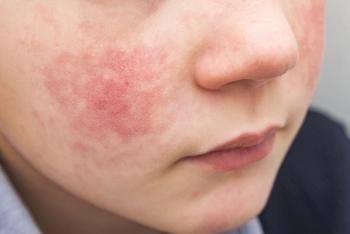
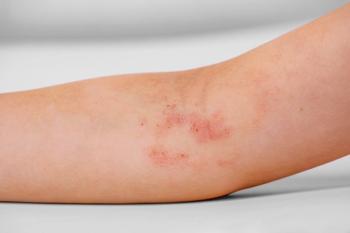
Brittany Craiglow, MD: Given the percentage involvement, do you think this patient warrants dermatology referral right away? Or do you feel she hasn’t tried that’s not over the counter, so the pediatrician tries triamcinolone twice a day for a couple of weeks to see what happens?
Angela J. Lamb, MD: She tried nothing but over-the-counter medication, so I’d probably go for a medium-potency topical steroid and then quick referral to a dermatologist. That’s mostly because of lifestyle. Sometimes the disease burden or body surface area is not directly correlated with how much is impacting somebody’s life. I’ll even take out that they talked about sleep. Sometimes kids are getting bullied, teased as if something is on the face—people start saying things. If there’s no clearance with that move quickly because of the lifestyle, then that needs to drive some of these decisions.
Brittany Craiglow, MD: That goes back to the treating the patient, right? For our initial discussion, as you mentioned, we talk with these families about what’s happening in eczema and gentle skin care. A lot of the families are doing everything right. They’re using a bland emollient. They’re not using soap or they’re using a soap-free cleanser. Sometimes I have families say, “I don’t understand. We’re doing Aquaphor every day, but she’s still itchy.” Talking about the barrier defect and all those things are important for barrier, but when you have inflammation, you could put moisturizer on until the cows come home and you’re still going to have itch. We have to treat the inflammation. Usually, the way we do that is topical corticosteroids, at least initially, but sometimes we get pushback with that. There’s this phobia about these medicines. How do you address that with your patients and their families?
Angela J. Lamb, MD: The use 2 phrases that stops it in its tracks. One, I tell people I would use these in my children. I have used them in my children. And 2, I tell them that it’s stressful to the body and raises internal cortisol for somebody to be itchy and stressed about their skin. The amount of cortisol involvement from the topical corticosteroids is so minimal compared with the stress of having itch and not being able to sleep. I like them to think about it like that. I find that tends to be a game changer. [Then I can] treat this child and put them out of their misery because it’s stressful. Itching is incredibly stressful to the family because it can create this power dynamic. The parent is telling the child to stop. I want to redirect them to focus on corticosteroids, which used under correct physician supervision do beautifully. People don’t have a lot of adverse effects. Research has been done on the amount of internal absorption—it’s fine, and there’s nothing with adrenals. But it’s very stressful. Your body’s internal cortisol is increasing when it’s stressed and you’re itchy and not able to sleep.
Brittany Craiglow, MD: It’s easy for a parent to view it as just a skin thing. But we have to remember the impact on the quality of life and other things, especially for young children. What does it mean for their sleep to be disturbed at a young age? There’s a lot of brain development happening. There’s still plasticity there. I sometimes say, “A lot of the calories your child is taking in are going to her skin. We want them to go into the brain, the kidneys, and other places where it’s more important.” We have to show that it isn’t just the skin. There are reasons beyond making them look less red or less itchy; that can be helpful. We also have to tell them that it’s not a forever thing. There’s an appropriate way to use these medications. If they become something that need to be used regularly, we’ve got to move on. We need to move up the ladder to a nonsteroidal, a topical steroid, or dupilumab.
Transcripts edited for clarity