Emergency Medicine
Latest News

Latest Videos

More News

Decreasing severe adverse safety events (ASEs) could improve the poor outcomes associated with children with out-of-hospital cardiac arrest (OHCA), since 60% had at least 1 ASE.

Leah K. Middleberg, MD, FAAP, explains her research on magnet ingestion and socioeconomic disparities, which was recently presented at the 2023 American Academy of Pediatrics National Conference & Exhibition.

The AAP recently updated their recommendations urging schools to be prepared for emergency medical situations including seizures, diabetes, allergies/anaphylaxis, mental health, substance use, or asthma.

Ahead of the US Senate Judiciary Committee hearing on gun violence prevention, the American Academy of Pediatrics announced the submission of a statement including more than 300 pediatricians sharing their personal testimonies on the subject.

While antibiotic dosing was correct, therapy duration was frequently inappropriate.

Does readiness to treat pediatric patients in the emergency department lead to less mortality in the year following presentation? An investigation offers answers.

Access to all forms of health care can be hard to find in rural areas. A new report examines how this impacts pediatric emergency medicine.

At the virtual 2021 Pediatric Academic Societies meeting, Niloufar Paydar-Darian, MD, attending physician at Boston Children’s Hospital, presented the results of a quality improvement program with the aim of eliminating serious preventable adverse events linked to discharge.

It's very likely that every medical provider will commit at least one medical error over the course of one's career. This infographic illustrates 7 common causes in emergency care.

Let’s continue to be vigilant in our practices to prevent medical errors, thus attaining what we all strive for: helping our pediatric/adolescent patients return to their normal thriving state of health and well-being.
A medical error is not an unusual event, although most are minor. The emergency department is one place where medical errors are more likely because of the chaotic nature. Here's a look at common mistakes and some cases where mistakes were made.
Are targeted screenings for sexually transmitted infections (STIs) or universally offered screenings more cost effective than not screening? An investigation offers some answers.

Identifying febrile children who have a life-threatening infection in an emergency department isn’t easy. An investigation looks at whether a new assessment can improve that identification.
Best practices for imaging in emergency departments has changed over the years. A new report offers a look at the trends in the past decade.
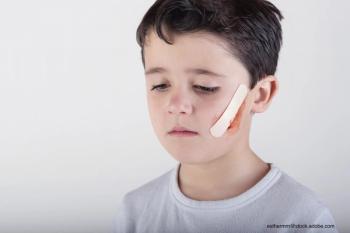
Not every child has a safe home. An investigation examines whether children with alleged maltreatment and who are at high risk of foster care placement have an increased risk of hospitalization for injuries.

Early warning scores have been shown to be helpful at determining children at risk of clinical deterioration. A report looks at whether an emergency department version of these scores could be effective.

Dizziness and sleep problems occur after concussions in young kids

Fractures are a fact of life for many children, but the COVID-19 pandemic has altered the activities of many children. A new report investigates the impact of the pandemic on the incidence of fractures.
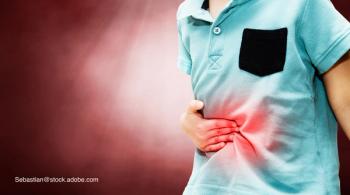
Algorithms and evidence-based guidelines have become increasingly used for treating gastroenteritis, but can they lead to better outcomes?
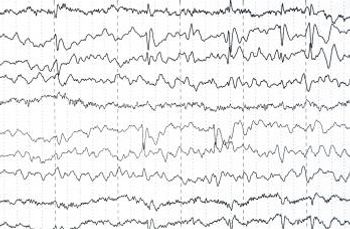
Many hospitals see pediatric patients who present with seizures in the emergency department, but a majority of cases that require admission are transferred to other facilities.

Children with mental health disorders are visiting emergency departments (EDs) at increasing rates. A new study looks at whether the EDs can provide optimal care.

A program at a hospital in New York City looked at how adding a pediatric observation unit to the existing pediatric emergency department helped improve patient outcomes and patient satisfaction.

A physician incentive program (PIP) that provides primary care providers (PCPs) with bonuses tied to specific goals to decrease pediatric emergency department (ED) use significantly decreases such visits, according to a retrospective analysis involving 1376 PCPs who participated in the PIP.
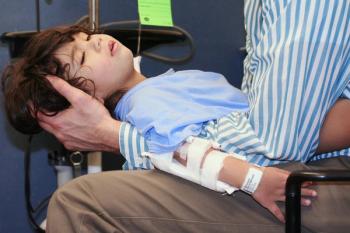
Pediatric patient revisit rates at emergency departments (EDs) have been historically underestimated, according to a new report, which includes revisits to other facilities.

Accidents happen, but many parents might take the opportunity to panic. Pediatricians can help them prepare.