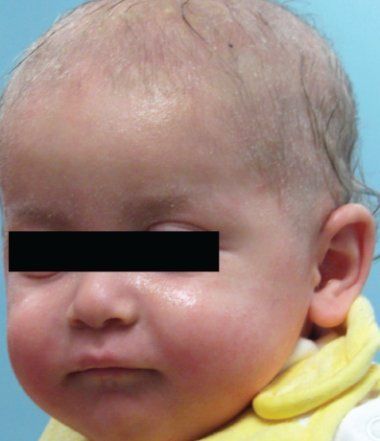
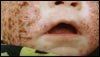
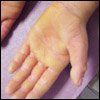
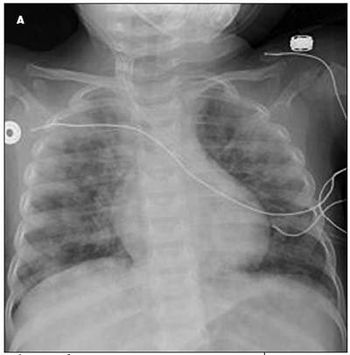
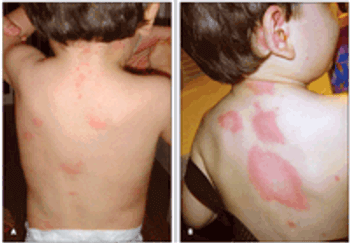
“Drug rash” is a common pediatric complaint in both inpatient and outpatient settings. This term, however, denotes a clinical category and is not a precise diagnosis. Proper identification and classification of drug eruptions in children are important for determining the possibility of-and preventing progression to-internal involvement. Accurate identification is also important so that patients and their parents can be counseled to avoid future problematic drug exposures.